Key Takeaways:
- Lichen planus symptoms often include purple or white patches on skin and mucous membranes, especially in the mouth and genital area.
- Triggers include viral infections, certain medications, stress and dry winter air that may worsen lesions.
- Diagnosis is clinical and sometimes requires a biopsy; treatment focuses on symptom control with topical steroids and good skin care.
- Seek a dermatologist if lesions persist, bleed or cause pain, as early assessment improves management.
White patches in mouth and genitals may signal lichen planus
Lichen planus is a common but often misunderstood inflammatory condition that affects skin and mucous membranes. While it typically appears as purplish, flat-topped bumps on the skin, lesions on the mucous surfaces such as the mouth and genital area frequently present as white patches. These signs can be alarming for patients, yet recognising the condition early helps clinicians manage symptoms and reduce complications.
Lichen planus symptoms and where they appear
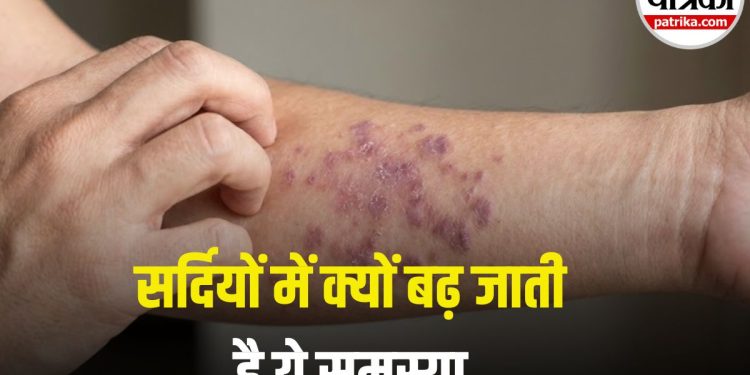
In many cases patients first notice a rash on the wrists, lower back or ankles. When the disorder affects mucous membranes, the appearance differs. Oral lesions may show as white, lacy patches or erosions that burn or bleed. Genital involvement often presents as white patches or thinning of the skin that can be itchy or painful. Nail changes and hair loss are less common but possible. Symptoms can worsen in cold, dry weather when skin becomes drier and more fragile.
Causes and common triggers
The precise cause of lichen planus is unknown; it is considered an autoimmune reaction in which the body’s immune system attacks cells of the skin and mucous membranes. Several factors are known to trigger or aggravate the condition. Viral infections, notably hepatitis C, certain medications such as some blood pressure drugs and non-steroidal anti-inflammatory drugs, and dental materials can precipitate lesions. Psychological stress and changes in the skin caused by friction or injury may also play a role.
How it is diagnosed
Diagnosis begins with clinical examination. A dermatologist will inspect the skin, oral cavity and genital area and take a detailed history of symptoms and medication use. Where the picture is unclear a small skin or mucosal biopsy can confirm the diagnosis by showing characteristic inflammatory changes. Blood tests may be ordered to exclude underlying infections such as hepatitis C.
Treatment and daily care
There is no cure for lichen planus but a range of treatments can control symptoms and promote healing. Topical corticosteroids are the mainstay for oral and genital lesions. In more severe or widespread cases systemic therapies such as oral steroids, retinoids or immunosuppressants may be considered. Good oral hygiene and avoidance of known triggers, including certain medications and harsh dental materials, help reduce flare-ups. During winter, use of moisturisers and a humidifier can protect the skin from drying out.
When to see a doctor
Patients should consult a clinician if white patches persist, cause pain, bleed, or if there are changes in sensation or function. Early assessment is important because chronic oral lesions carry a small risk of malignant change and require regular monitoring. A dermatologist or oral medicine specialist can advise on appropriate treatment and follow-up.
Awareness of the typical presentation helps patients and clinicians identify lichen planus promptly. Timely diagnosis and tailored management reduce discomfort and improve quality of life for those affected.